4 Priorities
Figur 4.1
Jim Goldberg/Magnum Photos/All Over
The Government will further strengthen Norway’s role in the global health efforts, with particular focus on three priority areas:
Boks 4.1 Health and the MDGs
Health has a prominent place in the UN Millennium Declaration from 2000 and the subsequent Millennium Development Goals. All eight goals are important for economic and social development, including good public health. Three of them relate directly to health: reduction of child mortality (MDG 4), improvement of maternal health (MDG 5) and combating HIV/AIDS, malaria and other diseases (MDG 6). The target of halving the proportion of people who suffer from hunger (1c), the goal of promoting gender equality and empower women (3) and the target of halving the proportion of the population without sustainable access to safe drinking water and basic sanitation (7c) are also important for health.
Mobilising for women’s and children’s rights and health
Reducing the burden of disease with emphasis on prevention
Promoting human security through health
The Millennium Development Goals are the main framework for Norway’s priorities in its health efforts. This means that we will focus on MDGs 4, 5 and 6, i.e. on child and maternal health, on children and young people and on combating communicable diseases. At the same time, the health aspects of the other MDGs and the scope of the Government’s engagement for global health indicate that a broader approach is needed. The efforts for disease reduction are focused on vaccination, communicable diseases, strengthening health systems, the health workforce, non-communicable diseases, food security, water, hygiene and sanitation. The last of these are also important for efforts to prevent climate change. The human security aspects dealt with in this white paper include these areas, as well as the integration of health objectives into foreign policy, pandemic preparedness, access to pharmaceuticals and the fight against sexual violence.
The Government’s position is that universal access to health services is important in order to reduce social disparities. We also attach importance to preventing discrimination based on sexual orientation and gender identity. In consequence, the Government’s policy also promotes access to health services for these groups, and the establishment of services geared to their needs.
4.1 Mobilising for women’s and children’s rights and health
4.1.1 Women’s and children’s health
Gender equality is crucial to achieving the health related MDGs. Women and girls must be able to visit clinics without the consent of family members. Economic barriers to services, including illegal part-payment and corruption, must be combated. Legislation on reproductive health must safeguard women’s right to contraception, provide protection against early marriage, violence and female genital mutilation, and establish the right to safe abortions. Norway will focus more strongly on the right to services and on measures that are particularly important for children, young people, women and vulnerable groups, including sexual and reproductive health and HIV prevention (see also Chapter 4.2.3).
Boks 4.2 Sexual and reproductive health and rights
Sexual and reproductive health means that people should be able to enjoy a responsible, satisfying and safe sex life, be able to reproduce and to choose whether, when and how often to have children. This implies that men and women have the right to be informed of, and have access to, safe, effective, affordable and acceptable methods of contraception, and access to suitable health services that allow women to go through pregnancy and birth safely and provide couples with the best possible conditions for having healthy children. Sexual and reproductive health also includes protection from and treatment of sexually transmitted diseases and other diseases and disorders connected to the reproductive organs and sex life.
Sexual rights include human rights that are already recognised in national legislation, international human rights instruments and unanimous declarations. For instance, they include the universal right of access to the best possible sexual and reproductive health services, sex education, respect for bodily integrity, freedom to choose whether or not to be sexually active, and the free choice of partners.
In addition to access to health services in general, family planning and professional midwifery services are critical components in the efforts to improve women’s and maternal health. Family planning is about the right of girls and women to make their own choices in the area of sexuality and fertility. It is also about efforts aimed at boys and men to change attitudes. Both teenagers and adults – women and men – should be guaranteed access to sex education and contraception. In many countries, domestic violence – including female genital mutilation, forced marriages and child marriages – is a significant underlying cause of high mortality and morbidity among girls and women. Early marriage and pregnancy often interrupt girls’ education and paid employment, and increase their vulnerability to HIV infection and disorders related to pregnancy.
Every year more than 273 000 women die as a consequence of complications related to pregnancy, and it is estimated that 15 % of women giving birth suffer potentially life-threatening complications. Qualified and motivated health workers in sufficient numbers are crucial, as are the infrastructure, equipment, guidelines and working conditions necessary to do a good job. It is the Government’s position that reproductive health also includes the right to safe abortions, and access to treatment in case of complications, regardless of the abortion’s legality.
Boks 4.3 Women’s rights and gender equality
The Action Plan for Women's Rights and Gender Equality in Development Cooperation affirms that «Norway will utilise international arenas, dialogue processes and programme support to raise controversial issues, and will advocate:
the decriminalisation of abortion and of women who have had illegal abortions, so that they can safely seek treatment if complications arise;
the decriminalisation of homosexuality and the fight to prevent all forms of discrimination and stigmatisation due to sexual orientation;
international acceptance for the concept of ‘sexual rights’, including the right to safe abortion on demand, and equal treatment regardless of sexual orientation.»
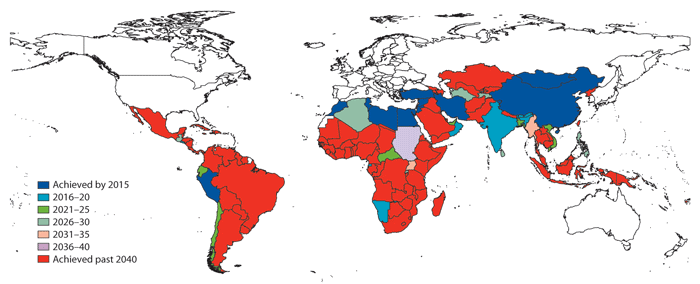
Figur 4.2 Millennium Development Goal 5 Improve maternal health, attainment year based on annualised rates of change, 1990–2011.
Kilde: The Lancet, vol. 378, issue 9797, 24 september 2011
MDG 5, «Improve Maternal Health», is the goal which is furthest from attainment by 2015. In the run-up to the UN summit on the MDGs in 2010, the UN Secretary-General launched the Global Strategy for Women’s and Children’s Health in order to increase focus on MDGs 4 and 5. The strategy concurs with the Norwegian emphasis on women’s and children’s health, and will provide a guideline for Norwegian priorities in the years to come.
The strategy focuses on the most vulnerable groups, such as pregnant women, newborn babies and young people, including the disabled, in the 49 poorest countries. Norway played a part in developing the strategy, and following it up will be one of the Government’s priorities.
The Minister of Foreign Affairs has participated in the Commission on Information and Accountability for Women’s and Children’s Health, which was created to improve global reporting, oversight and accountability in the field of women’s and children’s health. Furthermore, Norway chairs the Innovation Working Group (IWG) which is engaged in the efforts on the strategy through cooperation with the private sector and NGOs to develop innovative solutions for improving child and maternal health. When it comes to HIV/AIDS, a key goal in this context is to eliminate mother-to-child transmission of HIV. A global plan within the UN framework was spearheaded by UNAIDS and the US President’s Emergency Plan for AIDS Relief (PEPFAR) and adopted in June 2011. Norway supports this plan. In the autumn of 2011, the UN Secretary-General launched the Innovating for Every Woman, Every Child initiative, which encourages new and more flexible ways of working, centred around partnerships between the UN and public, private and civil society actors in the poorest countries.
The Government will:
Strengthen the access of women in the poorest countries to basic health services, including family planning, safe and de-criminalised abortion, safe delivery and innovative use of new technology;
Be at the forefront of the work to support sexual and reproductive health and rights, and universal access to health services;
Help to change attitudes where necessary to give vulnerable groups the same access to health services as others;
Emphasise the importance of midwives, and promote the training of more midwives;
Support competence-building measures for health workers in the treatment of victims of domestic violence and other types of sexual and gender-based violence, primarily through WHO, UNFPA and UNAIDS;
Increase the efforts against female genital mutilation through preventive work and awareness-raising campaigns, both in Norway and internationally;
Support efforts to change the attitude of men and boys regarding violence against women; and
Support research to increase knowledge about how sexual and reproductive rights and universal access to health services affect the general health situation.
4.1.2 Children’s and young people’s health – investing in the future
The right to life, survival and optimal development is a guiding principle in the UN Convention on the Rights of the Child. Chronic and acute malnutrition among children, low birth weight and insufficient breastfeeding cause an estimated 3.5 million deaths among small children under five, i.e. one third of all deaths in this age group. At least 200 million children under the age of five fail to develop to their full potential, with severe consequences both for the individuals concerned and for society as a whole. Early childhood is the most important period for all development. This is when the foundation for future education and work is laid, and it is possible to reduce the risk of malnutrition, obesity, mental problems, heart disease and social problems later in life. Investing in the first years of life is one the most important ways of reducing health inequalities. The potential effect of nutrition measures directed at children and mothers is great. For instance, infant mortality would be reduced by 13 % if the WHO guidelines on breastfeeding were followed.

Figur 4.3 Millennium Development Goal 4 Reduce child mortality, attainment year based on annualised rates of change, 1990–2011
Kilde: The Lancet, vol. 378, issue 9797, 24 september 2011
Adolescence is, with the early childhood years, a key phase of life for personal development and future health and wellbeing. There are more young people in the world than ever, and health threats like tobacco, misuse of alcohol, obesity and unsafe sexual behaviour are on the increase. This suggests that the health and education sectors are particularly important for protecting the rights of young people, and for building stable and sustainable societies.
Boks 4.4 Nutrition and the MDGs
Eradicate extreme poverty and hunger (MDG 1) – One of the indicators for this goal is the «prevalence of underweight children under five years of age».
Achieve universal primary education (MDG 2) – Malnutrition, particularly deficiencies in micronutrients, like iodine, is detrimental to children’s mental development. It reduces their possibilities for learning, and for completing their schooling.
Promote gender equality and empower women (MDG 3) – As a main rule, women play a key part in the provision of food and nutrition. They breastfeed, grow food, buy, cook and distribute the family’s food. Women also provide care, consult health services, and ensure good hygiene.
Reduce child mortality (MDG 4) – Every year one million children die from acute malnutrition. Malnutrition is an underlying cause in more than half of all deaths among children under the age of five, since common childhood diseases are often fatal in undernourished children.
Improve maternal health (MDG 5) – Malnutrition is a contributing cause of maternal mortality, ill health and complications during pregnancy and birth.
Combat HIV/AIDS, malaria and other diseases (MDG 6) – Malnutrition increases susceptibility to disease, and this in turn increases the need for nourishment and reduces the body’s ability to absorb nutrients. A balanced diet and good nutrition is therefore important for treating HIV patients for instance.
Ensure environmental sustainability (MDG 7) – It has been found that public health and the environment have a mutual influence. A sustainable environment and sound food production are important for ensuring good nutrition and sustainable management of biological diversity.
Develop a global partnership for development (MDG 8) – Nutrition involves many sectors and sustainable improvements depend on efforts involving actors with different backgrounds from a variety of institutions. Thus, nutrition is a good point of departure for promoting a partnership for development.
The health needs of children vary with age. This means that it is important to take a life-cycle approach to health. The UN’s Committee on the Rights of the Child has published two General Comments dealing with health, one on early childhood, and one on young people. General Comment No. 7, «Implementing child rights in early childhood», stresses that all states «should ensure that all children have access to the highest attainable standard of health care and nutrition during their early years, in order to reduce infant mortality and enable children to enjoy a healthy start in life». General Comment No. 4, «Adolescent health and development in the context of the Convention on the Rights of the Child», emphasises the importance of the right to health of young people as distinct from that of small children.
Particularly for girls, adolescence is a vulnerable period. Often, it is then that sex discrimination begins in earnest, and opportunities to continue their education or choose an occupation are limited through early marriage, early pregnancies, traditional demands to work in the home, and violence in the local community or as a consequence of conflict. According to UNAIDS, young people (in the age group 15–24) account for 41 % of new cases of HIV infection in the over-15 age group. More than 60 % of people living with HIV are girls and women. This has direct consequences not only for those affected, but also for their children. It is well documented that the mother’s age, level of education, health and nutrition are of crucial importance to child health and development.
There are particular challenges in the field of sexual and reproductive health. In many countries, young people do not have access to sex education, HIV testing and contraception because of cultural norms, stigma or legislation. NGOs play a crucial part, but since only one third of young people, according to UNAIDS, have adequate knowledge about the transmission of HIV, increased efforts are needed. It is important to raise awareness of the fact that providing sexual and reproductive health information and services for young people does not increase sexual activity and high-risk behaviour, but rather reduces unwanted pregnancies and HIV infection, and improves health.
The Government will:
Support efforts to prevent child marriages and teenage pregnancies;
Give priority to vaccination programmes to prevent disease, save lives and reduce infant mortality;
Facilitate the participation of young people in international dialogue and decision-making processes on matters related to their health;
Highlight the connection between nutrition and health, and strengthen the work in this area; and
Seek to foster greater acceptance in the international community of the need for and the benefits of sex education for young people as a preventive measure against the spread of HIV/AIDS.
4.2 Reducing the burden of disease with emphasis on prevention
4.2.1 Vaccination
All countries have now introduced child vaccination programmes. This has led to a substantial reduction in mortality. Nonetheless, more than 1.7 million children die every year from diseases that can be prevented by vaccination. Hence, vaccination is a vital strategy for achieving MDG 4, reducing child mortality.

Figur 4.4
Tor Aasgaard Borgersen/Office of the Prime Minister
The global alliance for vaccination and immunisation, GAVI, which was launched in 2000, is a partnership between the private and public sectors to improve access to vaccines in poor countries and contribute to establishing programmes for routine vaccination. WHO, UNICEF and the World Bank are key partners, and their efforts are important for achieving results. Norway was one of the initiators of the alliance, which is one of the most important channels for the Government’s efforts on global health.
In its strategy for 2011–2015, GAVI has set the goal of facilitating the vaccination of 250 million children and thus preventing 3.9 million deaths by 2015. The strategy includes the introduction of new vaccines, for instance vaccines against diarrhoea in children and cervical cancer in girls and women. In 2011, the Government decided to increase its funding to GAVI to the level of NOK 1 billion a year from 2015. An important aspect of GAVI’s efforts is the inclusion of measures to build local and national health systems. Experience from this work shows that targeted health efforts can be designed to bolster the development of general health services as well.
Securing a supply of effective vaccines at affordable prices in poor countries is one of the Government’s priorities. This is a complex area that is closely linked to efforts to strengthen health systems, cf. Chapter 4.2.3, and to patent rights and trade agreements in general, cf. Chapter 4.3.3.
Through its support for health research and innovative funding mechanisms, the Government has highlighted how the development of vaccines for instance against HIV and malaria has market potential in developing countries. Support is given to schemes to establish predictable demand in developing countries – based on the needs of the population – and stimulate research and development of effective vaccines at affordable prices in those countries. The need for publicly initiated research geared to the needs of developing countries is great, not least in those developing countries where the middle classes are growing rapidly. The pharmaceutical industry plays a complementary role, and should be given incentives to broaden its concept of market and increase its willingness to take risks. It is also a goal to increase production of vaccines in developing countries, for instance through cooperation with Norwegian research communities.
GAVI has a differential pricing policy that gives the poorest countries the lowest prices. It is the Government’s position that vaccine prices can be lowered further, and it is engaged in efforts to this end. The Government attaches importance to continuing and following up efforts in this area, including the work on GAVI’s new strategy process.
The Government will:
Continue its political, technical and financial support for GAVI to help introduce new, effective vaccines, and strengthen health systems and price competition in the vaccine market to benefit developing countries;
Contribute to the development of new mechanisms and new knowledge to improve access to vaccines for poor countries, including through research cooperation;
Continue the fight against polio and measles through awareness raising and economic support, with emphasis on the countries with the greatest burden of disease; and
Work in a coordinated manner through the relevant mechanisms to improve access to vaccines and strengthen production capacity in developing countries.
4.2.2 Communicable diseases – AIDS, tuberculosis and malaria
AIDS, tuberculosis and malaria – diseases included in MDG 6 – are among the ten leading causes of death in low-income countries, and are a priority in the Government’s efforts to combat communicable diseases. AIDS and tuberculosis are among the most important causes of death among women of fertile age in low-income countries, and many are infected with both diseases.
The Global Fund to Fight AIDS, Tuberculosis and Malaria is the most important channel for Norway’s funding related to MDG 6, and has been allocated NOK 450 million per year for the period 2011–2013. Support for the international drug purchase facility, UNITAID, is also part of this effort. UNITAID is an innovative financial mechanism. Its goal is to mobilise funds from a far broader donor basis than Europe and North America through the establishment of national taxes on domestic airline tickets. Other infectious diseases also cause a high burden of disease in poor countries. Many of these diseases, for instance diarrhoea in children under five, can be prevented and treated by simple means. This is one of the most important areas for UNICEF’s efforts, and Norway, among others, gives substantial support.
HIV/AIDS
The UN’s High-Level Meeting on AIDS in June 2011 marked 30 years of engagement with this disease. The last few years have seen a reduction in the number of new cases worldwide, not least because of the work of the Global Fund, which provides more than one third of the global funding for HIV/AIDS. At the High-Level Meeting, many countries reported good results in both prevention and treatment, but for every person being treated with anti-retroviral drugs, two new cases arise. This fact, combined with a tighter budget situation in many traditionally strong donor countries, means it is crucial to maintain political focus on the issue of HIV/AIDS. The Political Declaration from the High-Level Meeting set out updated targets for 2015 including halving the number of new cases from syringe sharing and sexual transmission, and eliminating mother-to-child transmission. It is also sets out the goal that 15 million people have access to HIV treatment by the end of 2015, an increase from six million today.
2011 marks the 25th anniversary of Norway’s active involvement in global HIV efforts. We have provided funding via multilateral organisations and NGOs, and have supported national responses. In addition, Norway has been actively engaged in global AIDS diplomacy to develop a good global response. The Government stresses the importance of integrated health services, which should include services related to HIV and AIDS. Integration with other reproductive and sexual health services is particularly important.
The rights perspective is central to the Government’s policy on HIV. Particular emphasis is given to women, children, young people and especially vulnerable groups, and their access to relevant services and information. Young people should play an active role in developing a response to the epidemic.
The group of especially vulnerable includes injecting drug users. In many countries, they account for a large proportion of new cases, and as they are often not given high priority by national health systems, reaching them presents special challenges. The United Nations Office on Drugs and Crime, UNODC, is responsible for HIV-related work in relation to drug users, particularly injecting drug users and prisoners. Norway supports UNODC’s harm-reduction efforts vis-à-vis drug users, for instance through access to clean hypodermic needles and medication-assisted treatment.
The Government will promote the rights of sexual minorities, gay, lesbian and transgender people. There is documented evidence that sections of the population that are the victims of discrimination are more vulnerable to and have a greater incidence of communicable diseases. Access to prevention and treatment is often difficult for these groups due to legislation and intolerance. This is not just a question of equal access to health services, but also a question of effective infection control. If treatment of HIV is started earlier, as WHO recommends, the risk of infection is reduced. Thus, treatment also helps in prevention.
The Government channels its HIV efforts through other multilateral partners in addition to the Global Fund, as well as through NGOs and bilateral aid. Norway will continue to play an active role on the boards of UNAIDS and UNITAID. The Swedish–Norwegian Counselling Team for HIV in Africa, based in Lusaka, Zambia, represents a coordinated approach to HIV/AIDS on a regional level.
Tuberculosis
One third of the world’s population is infected with tuberculosis, and 5–10 % of those infected develop the disease during their lifetime. The incidence of tuberculosis is in decline after a peak in 2004, but the decline is still too slow. Most cases are occurring in South-East Asia and Africa. In Africa HIV is an important factor in the tuberculosis burden. In Russia, the CIS states and East and Central Europe multi-drug-resistant tuberculosis is the greatest challenge.
The number of persons treated has increased substantially, and of the 22 countries with the highest incidence of tuberculosis, over half are now on track for achieving MDG 6. The Global Fund is by far the most important channel for funding efforts to combat tuberculosis, and is also an important channel for Norwegian funds. The Government supports WHO’s tuberculosis strategy by allocating additional funds to WHO. Norwegian research communities are involved in various aspects of tuberculosis research, and several Norwegian NGOs are also active in the field.
Boks 4.5 Vaccines and pharmaceuticals against communicable diseases
Both treatment and prevention are necessary to combat communicable diseases. Good vaccines are the most effective means of preventing a number of infectious diseases. Substantial challenges are involved in developing vaccines against the communicable diseases with highest priority, like malaria, tuberculosis and HIV. Also, only a limited range of pharmaceuticals are available to combat many of the most common infectious diseases. The extensive use of antibiotics and antiviral drugs has led to an increasing problem of bacteria and virus resistance.
The development of an HIV vaccine is a major undertaking, and substantial resources have been invested over several decades. Product development is demanding in terms of know-how and resources, and experience shows that developing a successful product is a time-consuming process. Consequently, such investments carry large risks. Development has been slowed down by lack of investment from both the private and the public sectors. However, in the last ten years, work on the MDGs has dramatically changed the situation, and increased focus on and funding of product development.
Norway participates in the European and Developing Countries Clinical Trials Partnership, an EU initiative for testing new vaccines against and methods of treatment of HIV/AIDS, malaria and tuberculosis through clinical trials on patients in sub-Saharan Africa.
The challenges in product development are multi-disciplinary, and are so great that no one actor can succeed alone. In order to meet these challenges and accelerate development, attempts have been made to strengthen cooperation through public–private partnerships. Product Development Partnerships (PDPs) are public–private partnerships that develop new technology and products geared to the health needs of poor countries. They coordinate and manage cross-disciplinary resources all the way from the research and development stage through to the introduction of products into the market.
The need for developing new products remains considerable, and requires long-term investment.
Malaria
Malaria has been found in 109 countries, but 35 countries, mainly in Sub-Saharan Africa, bear more than 85 % of the disease burden. Malaria is the cause of nearly 900 000 deaths a year. Four fifths of these are children under five. The disease is combated through the use of mosquito nets, indoor insecticide spray and pharmaceuticals in combination.
During the last five years, 34 countries have significantly reduced the number of cases. More than 600 000 children have been saved from dying from malaria. This is related to a strong increase in available resources for combating malaria through the global partnership Roll Back Malaria and the Global Fund, combined with access to more effective pharmaceuticals and mass distribution of mosquito nets. The Roll Back Malaria partnership has led to a better and more coordinated effort against malaria, and today it has more than 500 partners. The Government will continue to support efforts to combat malaria, primarily through the Global Fund and UNITAID.
The Government will:
Contribute to efforts to combat HIV globally;
Strengthen efforts and research related to communicable diseases in developing countries, with an emphasis on building capacity and competence. This includes strengthening the capacity of national health systems to carry out preventive work;
Further develop broad partnerships between multilateral organisations, national institutions, the private sector and civil society to combat communicable diseases. This includes organisations of those affected by these diseases, and cross-sector efforts, with particular focus on the link between HIV and tuberculosis;
Help to improve living conditions and quality of life for HIV-positive persons, and to normalising their status in society;
Continue to give priority to HIV/AIDS efforts with an emphasis on the rights perspective and the prevention and elimination of mother-to-child transmission; and
Promote the rights of vulnerable groups, including the decriminalisation of homosexuality, highlight the links between sexual and reproductive rights and HIV infection, and encourage national health systems to give due emphasis to HIV infection among injecting drug users.

Figur 4.5
UNICEF
4.2.3 Health systems
The concept «health system» involves all activities in a country whose purpose is to promote, restore and maintain health, including policy design, administration, management, financing and capacity for service provision. Efforts to improve health systems are facing challenges in all countries. In many of the poorest countries, a lack of resources, often combined with low political priority, problems of governance and inefficient management, is having a negative effect on the general health situation. This results for instance in weak maternal health, major disparities in terms of access to health services, high child mortality and inadequate vaccination coverage.
It is not possible to strengthen health systems unless national authorities shoulder their responsibility and establish policies that promote health, reduce health disparities in the population, and ensure universal access to health services. In this perspective, individual measures alone will be inadequate. Long-term, coordinated and systematic efforts are needed in several policy areas. Efforts in areas that bear directly on health, like health behaviour and the use of health services, must be supported by for instance an effective redistribution policy, good conditions for children to grow up in, and healthy work and living environments. It is therefore important that the health sector is able to engage in cross-sector efforts and to influence other sectors to ensure that they too are accountable for public health.
To build and maintain a national health system of this kind, a country needs a well-functioning education and research sector, with the capacity to train health workers of all categories, and to produce health knowledge to meet national needs in a wide sense.
Health system issues have to be addressed in order to take a comprehensive approach to health issues. From a development perspective this entails building capacity for supplying a broad spectrum of services. This again requires investment in effective national health systems, including fundamental factors like infrastructure, management, financing, health workers, pharmaceuticals and equipment, as well as systems to monitor public health, information systems and good governance. Taken together these elements lay the foundation for effective, universal health services covering a broad spectrum.
Since 2000 as many as 27 low-income countries have moved into the category of middle-income countries. The majority of very poor people do not live in the poorest countries, but in middle-income countries. The poor who live in these countries have not benefited from economic growth on a par with the rest of the population. It is also cause for concern that economic growth is not accompanied by a corresponding growth in the national health budget. Problems relating to weak health systems and unequal access to health services are no longer only due to unequal distribution between countries, but are increasingly also a question of unequal distribution within countries.
It is especially important that the general design of health systems in all countries pays particular attention to the health needs of vulnerable and marginalised groups, including indigenous peoples, migrants and the homeless, as well as the disabled, particularly women and children, many of whom do not benefit from global health efforts.
Health system problems clearly bring to the fore challenges relating to governance. Good governance is vital for all aspects of a health system. It is therefore crucial that efforts to build health systems take these interconnections into account. For example, the principle of zero tolerance for financial irregularities is always applied to the use of Norwegian funds.
Boks 4.6 Good governance
Good governance involves well-functioning political, administrative and service-providing institutions, and includes public participation in decision-making processes, democracy, the rule of law and transparent institutions. National health systems must have legitimacy and the confidence of the population. Good governance is a prerequisite for this. Good public health requires political understanding of the population’s needs, and the capacity to translate this understanding into political decisions across sectors. These decisions must also have the support of regional and local authorities. Not least when it comes to preventive work, mutual trust is of crucial importance. Access to health services for vulnerable groups cannot be guaranteed through international standards alone; it is also necessary for the interests and rights of these groups to be promoted politically at both national and local level. This presupposes civil rights and a functioning democratic culture.
The Government will continue to give priority to strengthening national health systems, with particular emphasis on prevention, primary health services and women’s and children’s health, especially through the World Bank, GAVI, the Global Fund and WHO. In addition, Norway plays an active part in the global coordination of the programmes for strengthening health systems in all these institutions, through the establishment of a common platform for funding health systems in the poorest countries. In addition to sector efforts, we also provide support for strengthening WHO’s normative and advisory work at country level.
Strengthening health systems is one of the priority areas in the global health efforts of the Research Council of Norway 2011–2020. Norwegian centres of expertise are making their mark in the field of health statistics and information systems.
The Ministry of Foreign Affairs is working on a strategy for cooperation with middle-income countries, and the global health aspect of this will focus on the obligation of national authorities to assume their responsibility for ensuring robust health systems that provide health services for all.
During the next ten years, health challenges will be affected by general development trends like population growth, economic changes, new political forces, increasing energy requirements, scarcity of natural resources and climate change. Health systems will also have to meet new developments at both local and global level that bring about changes in disease patterns. Key challenges include the prevention and treatment of non-communicable diseases, adaptation to climate change, and increased urbanisation. More frequent and more serious weather-related disasters, infectious diseases in the aftermath of such disasters and malnutrition as a result of changes in patterns of food production can be expected to put further strain on health systems.
The Government will:
Continue its political mobilisation efforts with a view to strengthening national governance and public management of national health systems;
Help to develop good public health systems that ensure access to primary health services, particularly for women, children and vulnerable groups in the poorest countries, for instance by urging the large multilateral organisations to give priority to this area;
Continue its work through WHO and the World Bank to develop sustainable financing mechanisms for health in developing countries that ensure robust health systems and universal access to health services;
Give priority to the prevention of both communicable and non-communicable diseases, and promote the development of health systems that are able to meet complex health challenges;
Promote stronger health systems for instance by the development and use of better health information systems and registries, the use of new technology and innovative solutions, health system research and collection of gender specific data;
Be at the forefront of efforts to persuade the major funds to invest even more in general strengthening of health systems;
Continue its focus on research on health systems and implementation research;
Continue its efforts to strengthen good governance, with emphasis on democracy-building, institutional development and the rule of law;
Continue to give priority to the fight against corruption throughout Norwegian foreign and development policy, with targeted efforts also in the health field; and
Ensure that Norwegian funds are managed in accordance with the principle of zero tolerance of financial irregularities.
4.2.4 Health workforce
The world faces a serious shortage of health workers, and several countries have problems covering current and projected needs for health workers. The challenge is definitely greatest in developing countries. WHO estimates that there is a shortage of nearly 4.3 million health workers worldwide. The shortage is most severe in poor countries. Although the need for health services varies between countries, most countries face challenges in covering current and projected needs for health workers. In many countries, it is becoming increasingly clear that training capacity is not able to meet current or projected needs for health workers. In addition, several countries, particularly developing countries, have health systems that are unable to absorb and make effective use of the workers that are available or are being trained. Countries in different parts of the world with different levels of development face different problems, but in many countries the situation is serious, and the provision of basic health services to the general population may be under threat. At the same time, many health workers migrate to work in richer countries where working conditions are better. The overall situation makes it legitimate to speak of a global health workforce crisis.
Most of the world’s health workers are in urban areas, whereas about half the world’s population lives in rural areas. It will not be possible to achieve equal access to services with the current geographical distribution of health worker resources. The Government therefore underscores that the realisation of the right to health for individuals presupposes a fairer and more uniform distribution of the health workforce.
Boks 4.7 The global health worker gap
According to WHO about 2.5 health workers (doctors, nurses and midwives) per 1000 people are needed to provide the population with a minimum level of essential health services. Fifty-seven countries fall below this threshold, and are consequently considered to suffer from a critical shortage of health workers. In these countries alone, WHO estimates a need for 2.4 million more health workers. The global health worker shortage is estimated at nearly 4.3 million. Particularly in sub-Saharan Africa the challenges are substantial, as a consequence of, among other things, a high disease burden, low training capacity and migration.
Health worker resources are very unevenly distributed relative to the burden of disease. For instance, Africa has 24 % of the global burden of disease, but only 3 % of the global supply of health workers, and only about 1 % of the funds allocated to health worldwide (including aid and loans).
The global health workforce crisis is a global problem and therefore requires global and comprehensive solutions. These solutions should be pursued through close cooperation and cross-border exchange of information. The global health worker shortage means that there is a great need for more training capacity globally, while the quality of training must be maintained. The expertise of practicing health workers must be maintained and developed in order to provide better services. It is also important that the distribution of work between the various categories of health workers matches needs and capacity as far as possible, and that the health worker training system takes this into account. Health workers are a scarce resource, and must be used as effectively as possible. This places demands on the quality and capacity for innovation of health systems.
Active recruitment from other countries is draining the poorest countries of health workers. In 2010, the member states of WHO agreed on the voluntary WHO Global Code of Practice on the International Recruitment of Health Personnel. This encourages high-income countries to combat active recruitment of health workers from countries with a critical shortage of health workers. The work on these guidelines is being followed up in WHO and in Norway. The Government decided that the health and care sector should implement the Code of Practice in 2011. Norway will thus refrain from active and systematic recruitment in poor countries where there is a shortage of health workers.
Preventing migration from poor to rich countries is important, but in many countries migration between rural and urban areas within a country also has negative consequences for the health system. At the same time, health workers must have the same right to move as everyone else. Efforts to avoid the negative consequences of migration must include improving local working and living conditions, which will help to prevent workers from leaving the sector, and supporting increased training of health workers with emphasis on high quality of training and services. Norway supports efforts to enable the poorest countries with heavy disease burdens to meet their needs for health system components like health workers, for instance through FK Norway’s exchange programme for health workers. Norway is also engaged in coordination efforts and investments that complement other international efforts to help solve the health workforce problems through coordination and investment.
The Government will:
Continue to develop a comprehensive approach to the health workforce crisis that takes into account considerations of both domestic and foreign policy in relation to recruitment, preventing the negative consequences of migration, and the training of health workers;
Actively contribute to the implementation of WHO’s Global Code of Practice on the International Recruitment of Health Personnel; and
Help to alleviate the health workforce crisis in poor countries, by supporting efforts to increase the number of trained workers and provide better working and living conditions for health workers, and by contributing to the development of innovative solutions to the health workforce challenges, including the distribution of work between different categories of health workers.
4.2.5 Double disease burden – non-communicable diseases
Non-communicable diseases, including cardiovascular diseases, cancer, chronic respiratory diseases, diabetes and mental disorders are the major causes of mortality globally. In low-income countries, other factors, like communicable diseases, complications in connection with childbirth and malnutrition still account for most of the life years lost, but here, too, non-communicable diseases are an increasing problem. In those parts of the world where infectious diseases still dominate, the growth in non-communicable diseases is a problem, as it adds to the existing burden of disease. Both are challenging health systems that may be poorly developed and have limited capacity. This creates what is often referred to as the «double disease burden». One of WHO’s 13 strategic objectives is «to prevent and reduce disease, disability and premature death from chronic non-communicable diseases, mental disorders, violence and injuries and visual impairment». A large part of this work takes place in developing countries.
Boks 4.8 Facts about non-communicable diseases globally
According to WHO’s Global Status Report on Non-Communicable Diseases, non-communicable diseases are the leading cause of death globally. Of the total number of deaths in 2008, 63 % were caused by non-communicable diseases, mainly cardiovascular disease, cancer and chronic respiratory diseases.
Almost 80 % of these deaths took place in low- and middle-income countries. These countries are also still severely affected by communicable diseases. The combination of communicable and non-communicable diseases therefore constitutes a double disease burden for these countries.
In the African region, there are still more deaths from communicable than from non-communicable diseases, but in this region, too, the incidence of deaths from non-communicable diseases is rapidly increasing, and it is estimated that non-communicable diseases will be the most common cause of death by 2030.
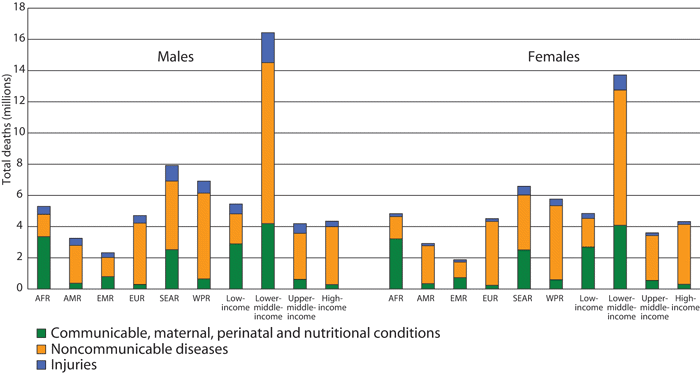
Figur 4.6 Total deaths by broad cause group, by WHO Region, World Bank Income Group and by sex, 2008.
Kilde: WHO: Global Status Report on Non-Communicable Diseases 2010
There is need for a targeted global effort in this area. Norway has good experience with preventive work, for example in the areas of tobacco and alcohol, taking a knowledge-based approach.
Unhealthy diets, tobacco use, harmful use of alcohol and physical inactivity are important risk factors for non-communicable diseases. It is obviously in the interests of the producers of tobacco, alcoholic and other drinks and foods to prevent the introduction of regulations that weaken the basis for their income too extensively. Norway’s position is that any potential conflict between commercial interests and health considerations should be clearly highlighted where appropriate. This implies that there are some contexts where the opportunities of private actors to influence the development of health policy should be limited. WHO excludes the tobacco industry from all forms of cooperation. Norway supports this line.
Mental disorders are given third place on WHO’s ranking of causes of the global burden of disease. In many countries, persons with mental disorders and their families are victims of systematic discrimination, and may be deprived of fundamental rights, like education, work and housing. The Government will promote greater openness about mental disorders internationally.
Reduction and prevention of non-communicable diseases is an important priority for WHO. It has developed a series of strategies, action plans and instruments for prevention and control. The main challenge now is to persuade individual countries to put the prevention of non-communicable diseases higher up on their national political agenda, for instance by becoming party to and implementing the provisions of the WHO Framework Convention on Tobacco Control, the WHO Global Strategy to Reduce the Harmful Use of Alcohol and the WHO Global Strategy on Diet, Physical Activity and Health.
Tobacco use is the single most important preventable cause of disease and death. The WHO Framework Convention on Tobacco Control, to which Norway is a party, establishes a legal basis for implementing effective measures to control tobacco.
Boks 4.9 The Tobacco Convention
The WHO Framework Convention on Tobacco Control is a knowledge-based, legally binding international treaty.
The Convention is the first international instrument on public health, and it entered into force in february 2005.
Gro Harlem Brundtland took the initiative for establishing the Convention in 1999, and this was a high priority during her tenure as Director-General of WHO.
As of september 2011, the Convention has 174 parties, and Norway was the first country to sign and ratify it.
Although a large number of countries have ratified the Convention, more needs to be done to persuade countries to implement the measures they have committed themselves to take. For instance, more emphasis could be given to taxation on tobacco products as a means of reducing use. This would also increase national tax revenues, which could then be used to implement further measures to improve public health.
The pace of implementation is also being threatened by actors in the tobacco industry, who have initiated legal proceedings against Norway and several other countries on the basis of international trade agreements.
The obesity epidemic is one of the main reasons for the attention that non-communicable diseases is attracting globally. Norway actively participates in WHO’s work in this area, and was a proponent of the WHO Set of Recommendations on the Marketing of Foods and Non-alcoholic Beverages to Children that were drawn up in 2010.
Norway has also participated in the preparation of WHO’s Global Strategy to Reduce the Harmful Use of Alcohol in 2010, and will continue its engagement in this field.
Developments in other policy areas, such as trade agreements and tax policy, also have a major effect on national policies on tobacco, alcohol and nutrition. This underlines the importance of integrating health policy issues into other policy areas, and of enabling national health authorities to work across sectors and influence cross-sector policy in their respective countries. Here, too, the development of effective regional cooperation is an important step towards global solutions.
The collective global efforts to promote health must take into account the changes in the patterns of disease. The fight against non-communicable diseases must be continued in relevant arenas such as WHO. Non-communicable diseases are also an important national concern for Norway, and it is important that the global and national efforts to respond to non-communicable diseases are designed to mutually reinforce each other.
In september 2011, the UN held a High-Level Meeting on Non-communicable Diseases, occasioned by the problems these diseases entail for health, national economies and socio-economic development. The most important outcome was the recognition that sectors other than health are affected by these diseases and must therefore be included in the efforts to combat them. The political declaration of the High-Level Meeting sets out that WHO, in cooperation with member countries, should «prepare recommendations for a set of voluntary global targets for the prevention and control of non-communicable diseases».
Prevention at the population level is a cost-effective means to combat the development of non-communicable diseases. Health systems must be able to provide services to populations with complex problems. Different systems and services are needed to treat people with non-communicable diseases than those needed to treat malnutrition and infectious diseases. Changes in the pattern of disease must be taken into account when designing and strengthening health systems. The collection and systematisation of national data on risk factors and disease burdens will be a natural part of this effort.
The Government will:
Follow up the WHO Set of Recommendations on the Marketing of Foods and Non-alcoholic Beverages to Children;
Seek solutions that build capacity for prevention in low- and middle-income countries. Primarily, this requires efforts at national level, but technical support from WHO and other UN bodies is also needed;
Seek to integrate non-communicable diseases into efforts to strengthen health systems;
Urge other countries to build a comprehensive public health policy based on the principle of «health in all policies»;
Help to expand the knowledge base through more research on and better systems for monitoring non-communicable diseases and risk factors in low- and middle-income countries;
Urge countries to ratify the Framework Convention on Tobacco Control and increase the pace of implementation;
Promote efforts to address non-communicable diseases in regional forums;
Help to increase knowledge and openness about mental health and psychiatric disorders; and
Urge countries to follow up their commitments to addressing non-communicable diseases, as agreed at the UN High-Level Meeting in New York 19–20 september 2011.
4.3 Promoting human security through health
4.3.1 Health challenges related to climate change
All population groups are affected by climate change, but the poorest are hardest hit, and are in a weaker position to meet these challenges. Climate change may undermine efforts to achieve the health related Millennium Development Goals (MDGs), and will create a severe additional burden for health systems that are already under strain because of insufficient resources.

Figur 4.7
Steve McCurry/Magnum Photos/All Over
There is a need for more knowledge about climate change and the consequences for health. In this connection, important lessons will be learned from the WHO and UNDP project on public health adaptation to climate change, financed by the Global Environment Facility (GEF). The project aims to «increase adaptive capacity of national health system institutions, including field practitioners, to respond to climate-sensitive health risks» in selected countries. The consequences for food and water supply and the risk of an increased geographical spread of communicable diseases are among the most predictable effects of climate change. The Intergovernmental Panel on Climate Change has estimated that an increase in temperature of 2.5 degrees Celsius in the next century will have dramatic consequences. There will be an increased shortage of drinking water and of water in general, an increased risk of famine and an increase in the spread of infectious diseases like malaria and dengue fever. In other words, robust climate change adaptation requires investment in health systems, with emphasis on prevention. It is important to underline that the health effects of climate change are additional to existing challenges, and the most severe impacts will be felt in some of the areas where the problems are already greatest.
Health is also clearly linked to global population development. There is good documentation indicating that low child mortality in a population leads to a reduction in the number of births. Improved reproductive health is therefore an important element in the efforts to address global population development.
Water, sanitation and hygiene
According to UNDP, more than half of all the sickbeds in the world are occupied by people with diseases linked to polluted water and inadequate sanitation. Hence, a six-fold increase in the risk of drinking water shortages will have enormous health-related, social and economic consequences. Diarrhoea kills 4 500 children every day, more than AIDS, malaria and measles combined. Nearly all deaths from diarrhoea (88 %) are caused by polluted water, inadequate sanitation and poor hygiene. Pollution is also an important health factor in other areas, for instance indoor air pollution caused by open fires and leaky stoves.
MDG target 7(c) is to «halve, by 2015, the proportion of people without sustainable access to safe drinking water and basic sanitation». Today, a quarter of the population of poor countries does not have access to clean drinking water, and nearly half does not have sanitation facilities. WHO and the UN’s Children’s Fund, UNICEF, have estimated that the economic returns on measures relating to drinking water, sanitation and hygiene are eight times the investment costs. In 2010, a UN Human Rights Council resolution affirmed «that the human right to safe drinking water and sanitation is derived from the right to an adequate standard of living».
The WHO/UNICEF Joint Monitoring Programme for Water Supply and Sanitation shows progress towards MDG 7 when it comes to drinking water. However, there are large regional and local differences. In sub-Saharan Africa, more than half the population does not have access to a satisfactory source of drinking water.
Globally, water is the nutrient that most people get ill from, and in the worst cases die from. Improving the water supply in a broad sense would have important health consequences. The link between drinking water, sanitation and hygiene will be emphasised in the Government’s global health work. Here, too, it is important to seek new alliances to strengthen global efforts.
Food security
Global trends like population growth, new patterns of consumption and use of crops (e.g. biofuels) and higher energy prices are putting an increasing strain on world food production. At the same time, food production is threatened by over-exploitation of natural resources, climate change, and pollution, for instance through the use of pesticides.
However, global food production today is sufficient to feed the entire world population. The fact that many suffer from malnutrition is therefore not only a question of production, but is also of social, political and economic factors that prevent food from being distributed equitably. The reasons for this include major inequalities in purchasing power, the low priority given to investment in the sector, and continued marginalisation of small farmers. The threats to food security are consequently complex, and are connected to several other policy areas.
According to the International Covenant on Economic, Social and Cultural Rights, access to sufficient quantities of safe and nutritious food is a human right (Article 11). At the UN World Food Summit in 1996, food security was defined in a broad sense as «when all people, at all times, have physical and economic access to sufficient, safe and nutritious food to meet their dietary needs and food preferences for an active and healthy life». Thus, food security also involves the provision of healthy and balanced nutrition as an important preventive health measure. Food security also requires efforts, both at national level and in connection with international trade, to ensure that food is safe from a health perspective.
The food supply situation and agricultural issues have received greater political attention as a consequence of the strong global rise in food prices. Nearly one billion people go hungry and suffer from malnutrition. Population increase, the development in the price of energy and other factors present substantial additional challenges to the efforts to achieve MDG target 1(c) on halving the proportion of people who suffer from hunger by 2015. A large proportion of the global potential for food production is lost because of poor processing and storage facilities, plant pests and animal diseases. Improvements in global hygiene and plant and animal health will significantly boost the efforts to supply the world with sufficient and safe food.
The Government will increase agricultural aid, and supports international and regional processes for agricultural development and food security, cf. the white papers Climate, Conflict and Capital1 and Towards greener development.2
Norway’s foreign policy will seek to safeguard food security between and within countries. States have an obligation to work towards enabling all inhabitants to provide for themselves. Where income and food supply are inadequate public social safety nets must be provided.
The Government will:
Integrate food security and climate change adaptation into efforts to promote global health;
Emphasise prevention in dealing with health challenges associated with the environment, urbanisation and climate change in developing countries by helping to strengthen the knowledge base for and research on these issues with a view to building competence and capacity in poor and vulnerable countries;
Actively promote, through WHO and other partners, stronger focus on the underlying factors for health, such as clean drinking water, sanitation, hygiene, nutrition and food security; and
Strengthen efforts on water, hygiene and sanitation through:
Preventive work at household level, with particular emphasis on hygiene,
The integration of drinking water, sanitation and hygiene into other sectors, including measures in schools and health institutions, and
The integration of the principle of the right to water into national legislation, and emphasis of the obligation of national politicians to give these issues priority.
4.3.2 Infection control and pandemics – prevention and management
In the white paper Climate, Conflict and Capital the absence of infectious, epidemic diseases is included as an important global public good that must be safeguarded through joint global efforts. The Government attaches importance to effective global pandemic influenza preparedness and response.
In 2005, the World Health Assembly adopted the International Health Regulations (IHR 2005). The so-called swine-flue pandemic (H1N1) in 2009 was the first serious test of these regulations. The subsequent assessment by an independent review committee shows that the regulations in general worked well during the pandemic, but that the world is ill-prepared to respond effectively to a serious pandemic or a similar international public health emergency.
Boks 4.10 Evaluation of the response to the H1N1 pandemic in 2010
In 2010, an independent review committee was given the task of evaluating how the International Health Regulations (IHR 2005) functioned during the H1N1 pandemic, and how WHO and its member states responded. Its brief also included proposing specific improvements that would strengthen preparedness based on experience gained during the pandemic.
The report concluded that the «IHR helped make the world better prepared to cope with public-health emergencies». Capacity at country level to detect, assess and report infectious diseases of importance to international public health is, however, still inadequate. The report recommends accelerating the implementation of the IHR and implementing measures to ensure that countries implement appropriate measures in a crisis situation as set out in the IHR.
The report further recognised that WHO had provided leadership and addressed several aspects of the pandemic well.
The committee concluded that «the world is ill-prepared to respond to a severe influenza pandemic or to any similarly global, sustained and threatening public-health emergency».
In 2011, the World Health Assembly adopted the Pandemic Influenza Preparedness Framework for a WHO-led response to future outbreaks of pandemic influenza. The framework accommodates the potential for improvement identified in the review of the H1N1 pandemic. This decision is historic and an important step forward for global health security, for international solidarity, and for WHO as an organisation. As co-chair of the process, together with Mexico, Norway played a prominent part in the challenging international negotiation of the framework, and, through painstaking diplomatic efforts, made a major contribution to a successful conclusion.
The objective of the Pandemic Influenza Preparedness Framework is to provide, under WHO leadership, a fair, transparent, equitable and effective system for sharing influenza viruses with human pandemic potential and for sharing goods, like vaccines. It aims to increase the global production of vaccines, with emphasis on establishing production in regions that do not today have such production capacity, strengthening laboratory capacity and improving access to vaccines and treatment for poor countries. The countries where outbreaks occur will be given priority. The pharamceutical industry is given a specific and formalised role, which includes providing both funding and products, within a legally binding framework.
WHO has established a programme to encourage the transfer of technology and know-how to developing countries, for instance by patent owners waiving their rights to allow production in developing countries. This should be stepped up, particularly in a pandemic situation. Under the framework, manufacturers of vaccines will be obliged to indicate whether they will sell their patent rights at affordable prices and completely refrain from asserting their rights during a pandemic with a view to facilitating production in developing countries.
The framework recognises that all states have sovereignty over their biological resources, and it is to be implemented in a manner consistent with applicable national and international legislation and obligations. Norway considers this to be in accordance with the aims of the Nagoya Protocol on Access to Genetic Resources, which has been adopted by the Conference of the Parties to the Convention on Biological Diversity.
Figures from WHO show that about 75 % of new infectious diseases, or known infectious diseases that have seen a strong increase in humans during the last 30 years are caused by pathogens from animals. The spread of various serious influenza viruses during the last few years is a clear example of how animal health and human health are closely interwoven. The challenges are particularly great in countries with high population density and close contact between humans and animals. Under the slogan «One World, One Health», WHO, UNICEF, the Food and Agricultural Organization of the UN (FAO) and the World Organisation for Animal Health (OIE) establish that understanding of the links between public health and the health of domestic and wild animals must be improved in order to meet serious health challenges in the 21st century.
Effective cooperation between FAO, WHO and OIE was consolidated through the global preparedness for avian influenza of the subtype H5N1 in the period 2004–2007. This work has provided an administrative and technical tool for a worldwide effort to combat animal diseases that may threaten public health. Norway has assisted this work through substantial contributions to various projects in these multilateral organisations. OIE has stated that the new hazards in the area of animal health can best be met by adapting «the existing systems of health governance at world, regional and national levels in a harmonised and coordinated manner».
The swine flu pandemic is an example of a serious communicable disease that can be transmitted between animals and humans (zoonosis). Among the most important preventive measures against such serious incidents of zoonosis are ensuring good standards of animal health, increasing awareness of the connections between public health and animal health, and strengthening cooperation between doctors, veterinarians and wildlife experts.
The Government will:
Support WHO’s efforts to implement and follow up the International Health Regulations (IHR 2005), and revise national and international plans in the light of the review of the H1N1 pandemic;
Support WHO’s work on the Pandemic Influenza Preparedness Framework and be a driving force in its implementation;
Contribute to raising awareness of the connections between public health, domestic animal health and wildlife health (One World, One Health); and
Help to strengthen international cooperation on access to effective pharmaceuticals and vaccines at affordable price.
4.3.3 Access to pharmaceuticals
The burden of disease is greatest, and health systems least developed, in developing countries. Developing countries have to a far lesser extent than developed countries been able to take advantage of innovations in pharmaceuticals and diagnostic technology.

Figur 4.8
John Vink/Magnum Photos/All Over
WHO has identified four key factors for access to pharmaceuticals: (i) affordable prices, including patents, (ii) rational selection and use, (iii) sustainable financing, and (iv) reliable health and supply systems. Although pharmaceuticals are in principle free in many developing countries, inadequate health services limit access in practice. This forces people into the private market, where availability is often far lower, prices higher and quality poorer. There are shortcomings related to all the four factors, not least in the regulations aimed at providing a reliable and stable supply chain. This is why the health system perspective is important (cf. chapter 4.2.3).
For a variety of reasons, many developing countries are struggling to build up adequate national expertise on the procurement of pharmaceuticals, and a financial basis to pay for them. A financial basis needs to be provided through taxation or other income. Furthermore, there are challenges regarding infrastructure for the rational distribution and use of pharmaceuticals in national health systems. On the institutional side, national pharmaceutical regulatory authorities are often a weak point. They have an important role to play in terms of quality control, issue of national licences and marketing permits, control and regulation of points of sale, and implementation of sanctions when regulations are not followed. This means that poor access to pharmaceuticals cannot be solved by national health authorities alone. The financial, legal and education sectors must also be involved and made accountable.
There are widespread problems relating to price levels, inadequate adaptation to patterns of disease, inadequate knowledge and transparency and weak planning. WHO plays an important advisory role in assisting in the choice of cost-effective pharmaceuticals. To facilitate efforts to improve countries’ general access to pharmaceuticals, WHO drew up the Essential Medicines List in 2001. This provides information on important and cost-effective pharmaceuticals that countries should buy to combat the major part of their disease burden. Only 5–10 % of the pharmaceuticals on the list at any one time are subject to patents. The rest are generic pharmaceuticals where patents are not a cost-driving factor. Patent rights, including patents on pharmaceuticals, are regulated in the Agreement on Trade-Related Aspects of Intellectual Property Rights (the TRIPS Agreement), which is part of the WTO rules.
At the international level, cooperation on the development of and access to effective and affordable pharmaceuticals is essential. It is important that this cooperation includes all parties, i.e. nation states, pharmaceuticals manufacturers, WHO, civil society and academia (cf. chapters 5.1 and 5.2).
Norway is active in several arenas in efforts to increase access to pharmaceuticals and diagnostic technologies. It is the Government’s position that WTO rules should not be applied in a manner that deprives poor countries of the autonomy and instruments that have been important in the development of our own welfare society. Norway will not make demands on poor countries that could undermine their ability to develop strong public services in the fields of health and education. Norway has emphasised that the TRIPS Agreement should not stand in the way of measures to protect public health. At the same time, it must be borne in mind that the patent system is important for the development of new pharmaceuticals. Based on these considerations, Norway was one of the driving forces behind the 2001 Doha Ministerial Declaration on TRIPS and Public Health and in the work to find a solution to the ban on the export of pharmaceuticals with a compulsory licence (generic production of pharmaceuticals – so-called copy-cat drugs – without the consent of the patent holder). The Doha Declaration from 2001 establishes that trade rules, including patent rules, should not stand in the way of public health concerns, and that countries should be allowed to use the flexibility of the TRIPS Agreement to safeguard access to pharmaceuticals.
In May 2004, Norway became the first country to amend its legislation to take advantage of the flexibility allowed under the TRIPS Agreement. Since Norway is only a small producer and exporter of pharmaceuticals, these amendments in themselves have little significance in terms of improving developing countries’ access to pharmaceuticals. Nonetheless, they confirm and reflect Norway’s positions in the international negotiations and processes on access to pharmaceuticals and patent rights. When the international drug purchase facility UNITAID was established in 2006, with Norwegian support, its mandate stated explicitly that it should help countries to make use of the flexibility of the provisions of the TRIPS Agreement and the Doha Declaration. Key pharmaceuticals-manufacturing countries, like the UK, Brazil and France, have agreed to this principle by becoming partner countries.
Effective treatment of HIV/AIDS has been available since the end of the 1990s, and increasingly effective pharmaceuticals are being developed. However, high prices have meant that developing countries could not afford them, or have chosen not to give them priority. One solution to this problem has been the establishment of major global financing schemes to give developing countries access to effective drugs, where the full range of actors – states, the UN system, the private sector, civil society and academia – are involved as partners. The Global Fund and GAVI are flagships in this connection. UNITAID is also important in this context. Within the framework of the patent system it will be important to continue efforts to develop new forms of collaboration to improve access to pharmaceuticals, such as UNITAID’s Medicines Patent Pool, which was created in 2010. The scheme lets patent holders place their patents in a «pool» that can be used by manufacturers in developing countries to produce pharmaceuticals in return for a fee and a percentage of their earnings from the product.
The development of pharmaceuticals for the diseases that are most common in poor countries is hampered by the fact that markets in these countries have little purchasing power and are too small for research and development to be profitable. In 2006, WHO established the Intergovernmental Working Group on Public Health, Innovation and Intellectual Property which resulted in a global strategy and a plan of action that were adopted by the World Health Assembly in 2008. Norway has continued its involvement in this work by leading the current working group on the selection of specific projects for research and development.
Based on a G8 initiative, Norway has, together with Canada, Italy, Russia, the UK and the Bill & Melinda Gates Foundation, established an innovative pilot scheme to help develop and produce a vaccine for pneumococcal disease. The scheme has helped to mobilise Russian engagement. Its basis in the G8 illustrates the importance of high-level political leadership (cf. Chapter 5.2).
The Government will:
Give priority to the work on strengthening the supply of pharmaceuticals to developing countries with focus on integrated health services and international initiatives and processes to create markets in developing countries;
Continue to support research and development in the field of pharmaceuticals for developing countries, with a focus on building and strengthening production capacity in these countries;
Promote innovative arrangements for improving developing countries’ access to effective pharmaceuticals that are available within the framework of the patent system, for example through broad partnerships between states, civil society, academia and pharmaceutical manufacturers; and
Work to reduce prices and establish global procurement schemes that improve access to pharmaceuticals for women and children, among others.
4.3.4 Sexual violence during and after conflicts
Civilian suffering in modern armed conflict is enormous. Women and children are particularly vulnerable to sexual violence in conflict situations. In a number of conflicts in recent years, rape and other forms of sexual violence have been used systematically as a weapon of war. In many cases, however, sexual violence is random and opportunistic, and a consequence of a breakdown of law and order in conflict and crisis situations. Prolonged violent conflict leads to a general brutalisation of society, and women and children are particularly vulnerable.

Figur 4.9
Jim Goldberg/Magnum Photos/All Over
Irrespective of the underlying cause, extensive sexual violence has a serious impact on health in the societies where it occurs, and – through migration – in other societies too.
The use of sexual violence in conflict is prohibited under international law. All parties to conflicts – both state and non-state armed groups – are obliged to follow these rules. International norms and case law have become more stringent. The UN Security Council has established that «rape and other forms of sexual violence can constitute a war crime, a crime against humanity, or a constitutive act with respect to genocide».
Norway has taken active part in the efforts to ensure that sexual violence is treated on a par with other threats to international peace and security, and that the experience of women in war and conflict is taken fully into account. Norway is strongly engaged in the follow-up to the UN Security Council resolutions on women, peace and conflict (S/RES nos. 1325, 1820, 1888, 1889, 1960). In recent years, the Government has increased its efforts to prevent and protect against sexual violence, increase the number of prosecutions, and improve rehabilitation services for survivors.
The health sector plays an important part in prevention, treatment and rehabilitation. Survivors need medical, psychosocial and economic rehabilitation, and such services are decisive for successful re-integration of victims of sexual violence and for reducing stigmatisation. Prevention of and response to sexual violence should be integrated into all plans to improve reproductive health in crisis situations. The health sector also plays a key part by documenting the incidence and extent of sexual violence, and in collecting evidence that can be used in the prosecution of perpetrators and their leaders. Preventive measures must include initiatives directed at men in general and their concepts of masculinity. Furthermore, there is a need to improve the quality and availability of data, and to foster political will to enact effective measures against impunity, particularly in countries where conflict-related sexual violence is common. The health aspect of conflict management is increasingly recognised, as reflected for instance in Security Council resolution 1983 (June 2011), which underlines the importance of incorporating HIV measures into the implementation of peacekeeping missions.
The Government will:
Work towards the integration of efforts to combat sexual violence in conflicts and improve services for victims into the Global Strategy for Women’s and Children’s Health, and to improve coordination of these efforts;
Seek to ensure that multilateral and global health schemes implement and support efforts to prevent and protect against sexual violence in conflict and post-conflict situations;
Seek to ensure that multilateral and global health schemes include conflict-related sexual violence in their dialogue and cooperation with national authorities, with a view to strengthening political commitment to prevention, treatment and rehabilitation; and
Support efforts to improve access to reproductive health services, including safe abortion and services for young people, during and after situations of conflict and crisis.
4.3.5 Health – foreign policy and international cooperation
Foreign policy must take health issues into account, and health issues must have a foreign policy dimension. The linkage between health and security has become more recognised internationally (for instance HIV/AIDS was on the Security Council’s agenda as early as 2000), but many challenges remain.
An effective global health policy entails relating to a broad spectrum of actors, and if necessary seeking new forms of cooperation. In 2006, Norway and France took the initiative to establish the Foreign Policy and Global Health initiative, which focuses on the links between these areas. It involves the foreign ministers of seven counties: Brazil, France, Indonesia, Norway, Senegal, South Africa and Thailand.
The network is well established, and has become well known not only in the health community, but also in the wider political landscape. It has come to be seen as an important, innovative and effective network, which is setting the agenda and promoting dialogue in the interface between foreign policy and health, primarily through multilateral processes and arenas in Geneva, and through regular reporting and debates in the UN General Assembly in New York. It is an arena for dialogue across regions and positions.
The work on promoting global health through foreign policy reaches beyond traditional health forums. Other international processes often have substantial consequences in the health area as well. Our positions in international forums on for instance trade, human rights, peace and security often have a considerable impact on health. Norway is not one of the largest international actors, but our positions, resources and willingness to help mean that we are often listened to. This is the case for instance in the negotiations on compulsory licensing to facilitate production of affordable pharmaceuticals, the positions we take in the WTO and in our engagement in common efforts to develop conventions that ensure the fundamental rights of all people in all countries.
The Mine Ban Convention (1999) and the Convention on Cluster Munitions (2008), in which Norway played a very active part, have had great impact on the health situation of civilians during and after armed conflicts. The UN Security Council has adopted two resolutions on HIV/AIDS and security (S/RES 1308 in 2000 and S/RES 1983 in 2011). These state that HIV/AIDS is a security threat since the pandemic kills productive members of society and may pose a risk to stability and security. They particularly emphasise the role of uniformed forces, the importance of HIV prevention and treatment among them, and the importance of ensuring that peacekeeping forces do not become a factor in the spread of HIV infection in the countries where they operate. Health work in connection with crises and conflicts is generally part of humanitarian efforts and is dealt with in the white paper Norway’s Humanitarian Policy.3 International processes that seek to promote economic or social development in any sense must include health as a fundamental element. Many of the most important preventive measures in relation to climate change are health-related, and many of the most serious impacts of climate change are in the health area. There is a need to strengthen understanding of these connections, particularly among political decision-makers globally.
The International cooperation on health is part of the Government’s global health policy, and it is vital to ensure that the connections between global measures and Norwegian public health are properly taken into account.
This cooperation takes place in a diversity of arenas. There is a tendency that international rules and regulations are becoming more binding. Norway’s commitments under international agreements on trade in products and services also have implications for our national health policy. EU rules on marketing, distribution and standards for foods, beverages and pharmaceuticals are binding for Norway under the EEA Agreement. This is also the case for the rules on migrants’ health and their right to health services, and for the Directive on standards of quality and safety of human organs intended for transplantation (the Organ Directive), which was adopted in the summer of 2010. A new EU directive on patients’ rights in connection with cross-border health services will also affect Norway. The EEA and Norway Grants have facilitated extensive cooperation with several EU countries in Central and Southern Europe in the areas of research and collaboration between health authorities. Through the WTO, Norway is under obligations in several areas that concern health, for instance through rules on patents and on trade in goods and services. For instance, Norway is an active participant in the Codex Alimentarius Commission, which develops international food standards.
The UN, and particularly WHO, is an important arena for health policy. Norway has committed itself to two legally binding agreements under WHO, the Framework Convention on Tobacco Control (FCTC) and the International Health Regulations (IHR, 2005). Norway is a party to the joint WHO and United Nations Economic Commission for Europe (UNECE) Protocol on Water and Health from 1999. The main aim of this Protocol is to promote health through improved water management, including the protection of ecosystems and the reduction of water-related diseases. At the Meeting of the Parties in november 2010, Norway was appointed to chair the Bureau for this protocol for the following three-year period. Norway is also engaged in the work of the United Nations Office on Drugs and Crime (UNODC).
The Nordic cooperation on health and food safety is an important arena for cooperation with our neighbouring countries in such areas as health services, food safety, preparedness, crisis management and border controls. The Nordic arena is an important platform for cooperation vis-à-vis the EU and WHO, and is also an example of how regional cooperation channels can be valuable supplements to global channels.
Today, antibiotics resistance is a rapidly growing problem, and constitutes a serious threat to global health. At the same time, the development of new antimicrobial pharmaceuticals has slowed down. It is therefore possible that we face a future without effective antibiotics, and that infections that today are regarded as harmless may again become a serious health problem and a major cause of death. The Nordic countries agree that antibiotics policy should be restrictive, and, under the auspices of the Nordic Council of Ministers, will cooperate on reducing the development of antibiotics resistance globally. The EU, too, has this issue high on its agenda, with the aim of slowing down the development of resistance.
Norway has a bilateral health cooperation agreement with Russia, and plays an active part in the regional health cooperation in the High North. This takes place primarily in the Northern Dimension Partnership in Public Health and Social Well-being and the Barents cooperation on health and social issues. The partnership works to improve the situation in the region, by combating communicable and non-communicable diseases and promoting a healthy life-style. Norway and Russia focus particularly on cooperation on measures to combat the harmful use of alcohol. Within the Barents cooperation, particular emphasis is given to HIV/AIDS and tuberculosis. The prevalence of these diseases is still worrying in parts of the region. Norway also has a bilateral health agreement with China, which is being followed up through a multi-year action plan, with particular emphasis on public health, prevention of disease, health system development, primary health services, infectious diseases (prevention and control) and global health.
The Government will:
Integrate a global health perspective into its general foreign policy;
Actively follow up the priorities of the Foreign Policy and Global Health initiative:
To highlight the health effects of foreign policy, and improve the promotion of public health nationally and globally,
To win acceptance for policies that promote public health and health security in specific health-related situations in a range of international health and foreign policy arenas, and
To build alliances and confidence through a cooperation on health that has ripple effects on wider foreign policy goals.
Highlight the connections between health and well-being, social development and security;
Work towards better coherence and coordination in Norwegian international health cooperation; and
Contribute to the work to develop a common European antibiotics policy to slow the development of antibiotics resistance globally.