3 Myths about care services and themes for the future
«We did not come to fear the future. We can here to shape it.»
Barack Obama
3.1 Future challenges for the care services
In Report No. 25 (2005-2006) to the Storting, «Long-term care – Future challenges, Care Plan 2015»», the Government identifies five future challenges for the care services:
Society is facing demanding challenges in the care services in the coming decades. These cannot be dealt with by the health and social services sector alone, but must be addressed on the basis of a public responsibility involving most of the sectors in society and by supporting and developing new forms of involvement and participation by the families and local communities, organisations and enterprises. As far as we can see today, the challenges will be related primarily to:
New user groups
Due to the dramatic rise in the number of younger users with reduced functionality and a wider array of health and social problems, the care services will need to incorporate a different type of professional expertise and an integrated life course perspective.
Ageing
The growing needs of a larger number of elderly will require an expansion in capacity and greater expertise on ageing, especially related to dementia and complex medical conditions. The scope of the challenges must nonetheless be viewed in light of the fact that the new elderly generation is better equipped to meet and cope with old age owing to its improved state of health and greater resources in the form of higher education and better financial situation.
Shortage of care providers
Due to changes in the age composition of the population, there will be no substantial increase in access to labour and potential volunteer care providers. A lack of growth in informal care means that the public sector must assume responsibility for the entire increase in needs that is anticipated, and will be dependent on locally based care services that cooperate more closely with families, volunteer care providers and local communities.
Medical follow-up
There is a need for better medical and interdisciplinary follow-up of recipients of public home care services and residents of nursing homes and residential care homes. This applies especially to people with chronic and complex medical conditions, dementia, mental health problems and others who have a need for coordinated services from both the specialist health care services and the municipal health and social services.
Active caregiving
Care services involving daily life, meals, activities, and social and cultural factors are identified in most studies as comprising the weakest services today. Improving these areas will require a greater breadth of professional expertise that includes a wider variety of professional groups so that the care services are able to meet users’ psychosocial needs and can be given a more active profile.
The committee has used these five main challenges as the basis for its activities, and refers to the analyses performed in connection with the Government’s Care Plan 2015 (Report No. 25 (2005-2006) to the Storting). The Government has also followed up the efforts related to these five challenges in its Care Plan 2015, which lays out a main strategy that utilises the upcoming period of relative demographic stability to:
plan and prepare for the rapid growth in the need for care services that is expected to occur in 10 to 15 years from now, and
gradually expand the care services by investing in preventive measures, education and competency building, new technology, housing and facilities.
In addition, the Government has drawn up the Coordination Reform to improve cooperation between the municipal health and care services and the specialist health care services. The committee has decided to explore those issues and needs not covered in the reform. In keeping with the mandate and on this basis, the committee has focused its efforts on assessing new approaches and solutions for meeting the caregiving challenges in a time horizon that extends beyond the Government's Care Plan 2015, putting special emphasis on technology, alternative living arrangements and forms of organisation, and research and innovation.
Moreover, the committee points to the challenges and opportunities inherent in these problems when viewed in an international context, where:
the personnel market is becoming internationalised, and the care services workers are increasingly exported and imported,
larger service providers operate in an international market,
growing numbers of patients and users are crossing national borders for treatment, recuperation and physical training.
The future outlook must also be viewed in light of the vast changes occurring in the age composition of the population in both Europe and the world at large. There is reason to believe that this will affect all markets and social sectors throughout the world. In this context, Norway is more fortunate in that it is experiencing less dramatic changes in this regard than the other countries in Europe. Society will face major challenges relating to care services in the coming decades. These will be demanding enough without being made worse by dire predictions and worst-case scenarios.
In the view of the committee, the future challenges for the care services cannot be dealt with by the health and social services sector alone by employing more professional staff, building more institutions and implementing new, formal assistance schemes. On the basis of a public responsibility, most sectors of society must help to further develop community-oriented solutions that are adapted to the new needs and available resources. It will be essential to support and develop new forms of involvement by volunteers from families and local communities, user-driven organisations and enterprises, based on interaction between the public sector and civil society. The issue at stake has just as much to do with the kind of society Norway seeks to build for the future as with how the health and care services sector will develop.
3.2 Five myths about care services
In order to address the future challenges of the care services, it has been crucial for the committee to obtain a clear picture of the current caregiving situation. Many ideas about this have been formed, partly from descriptions in the media and partly as a result of the particular focus in the public debate at the national level. It has been important for the committee to clear away some of the misconceptions that have long been associated with the care services sector and to obtain an up-to-date picture by using relevant data and research in the field.
3.2.1 The myth about elderly care
The municipal care services are no longer for the elderly only. They cover the entire life course and offer services to families with children, adults with reduced functionality and elderly with serious illnesses and loss of functionality. Services are provided in all types of dwellings, from homes for disabled children with a great need for assistance to residential care homes and nursing homes, although most of the people receiving care services are living in their own homes.
In the public debate, however, the care services are often discussed as if they were synonymous with elderly care. The media and participants in the public debate often measure the success of these services in terms of the number of nursing home beds. The actual situation is far more nuanced. While only about 40 000 people receive care services in nursing homes, 225 000 people receive care services in their own homes or in residential care homes. One-third of these are under the age of 67.
Twenty years ago, two-thirds of the care services resources were used in homes for the aged and nursing homes, while only one-third was used on home care services. Today more than half of the resources in the sector go to home care services and measures outside of institutions (Brevik 2010).
The fact that the municipal care services have recipients of all ages with a variety of needs, both with regard to the type of living arrangements and the services offered, is often left out in discussions of nursing homes versus residential care homes and institution-based services versus home care services.
This is why the concept of «elderly care» does not figure in health and social services legislation or in the national or municipal budgets. The statutory framework and access to resources are primarily based on the principle that age must not be used in a discriminatory fashion. The care services therefore encompass everyone who has a need for them, regardless of age, gender, diagnosis, level of functionality or problem.
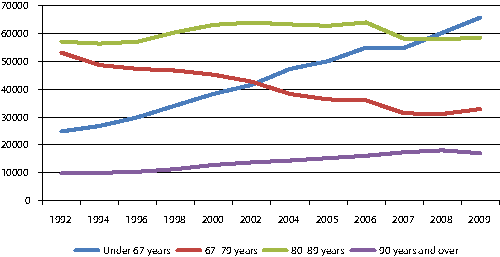
Figur 3.1 Number of recipients of home care services by age. 1992-2009
Kilde: Statistics Norway. See http://www.ssb.no/pleie/ (in Norwegian only)
The idea that the municipal care services are synonymous with elderly care has become less and less correct over time. In fact, in the past 20 years the number of elderly users of these services has not grown, while the number of users under the age of 67 has tripled in the same period. Almost all of the new resources invested in the sector in recent years have gone to covering the growth in the younger user groups.
Despite the strong growth in the oldest age groups in recent decades, the number of elderly users of homes for the aged and nursing homes has not increased. Thus developments are not only being driven by ageing, but are also influenced by other changes in society and the shift in the distribution of tasks which has occurred over time between the specialist health care services, informal care providers and the municipal care services. In this context, the municipal care services fall right in the middle between the special health care services and informal care providers, and have a broad scope of interaction with both areas.
The committee sees the importance of continuing to ensure that care services are provided to everyone regardless of age. More than ever before, it is crucial to build a foundation for the welfare schemes that is based on support from young and old alike and that encourages solidarity between the generations. Equal rights to services for everyone with a need, regardless of age, is a basic principle underlying mutual understanding and joint responsibility.
The services must nonetheless be adapted to various phases of life and to the individual’s particular resources and needs. The services provided to a younger user with reduced functionality who requires assistance to complete an education or to gain employment may therefore be different than the services provided to an elderly couple where one of them has developed severe dementia. In one instance, the main focus will be the person's potential to live an independent life, relying as little as possible on others. In the second instance, the need for safety and protection will be more important, even if it comes at the expense of independence.
With regard to the use of new technology and advanced technical aids, younger people with reduced functionality are at the vanguard in the development of this sector precisely because these advanced technical aids help individuals to cope better with daily life on their own and be independent of others. There is reason to believe that the new generation of senior citizens will follow suit, given their attitudes towards independence and control over their own lives. Since the care services sector has limited historical experience with applying new technology, it is the users themselves who will more often be the driving force behind innovations and the implementation of such technology. Demand from a much larger user group with greater buying power will also probably create a basis for more market-based services.
Given how care services evolve, there is great potential for new solutions for the traditional care services to elderly users to be found in transferring the experience gained from reforms implemented for other user groups. For example, the reform for people with disabilities showed that it was possible to establish effective 24-hour services outside of the institutional framework. The reform also encouraged other sectors to take responsibility for people with disabilities on par with the rest of the population with regard to everything from education, employment, activities and transport to participation in cultural events and sport. In the view of the committee, these should be key objectives for the development of care services in the future.
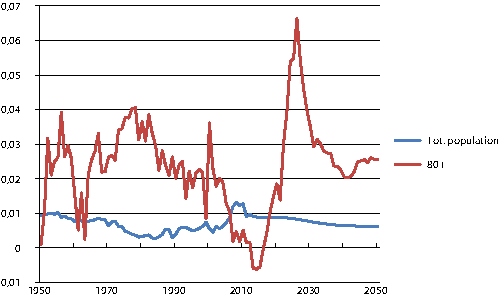
Figur 3.2 Percentage change from the previous year in the number of persons 80 years or older and for the population as a whole. 1950-2050
Kilde: Statistics Norway 2010 Population projections, median alternative
3.2.2 Myth about the «elderly boom»
The demographic changes facing society are often depicted as an unchecked «elderly boom» about to inundate the world. Crisis scenarios are being applied to pension systems, the labour force and the lack of health and social services workers, and dramatic projections are being made about the extent of illness and caregiving needs among the population.
However, the «elderly boom» will be demanding enough without painting the blackest picture. The committee takes a more moderate view of the impact of the changes that will occur in the age composition of the population, and identifies certain factors that will mitigate the challenges facing Norway, especially in the area of care services:
The number of elderly over 80 years of age will not increase in the next 10 to 15 years. Since a substantial share of the resources in the care services sector are dedicated to the 80+ age group, Norway now has a «demographic moratorium» or «breathing room» (Barstad 2006). This period should be used to prepare and plan for the dramatic increase in this age group that will occur from 2025 onward (Fig. 3.2).
In terms of demographics, Norway is the country in Europe that will experience the fewest dramatic changes in the age composition of the population, in part because Norway has already undergone such changes and in part because Norway has a higher birthrate, so that ageing is combined with continued population growth. The Potential Support Ratio shows the relationship between the working population (16-66 years) and the elderly population (67 years and older), and is of great interest with regard to the financing of pensions, welfare services, and health and social services. Figure 3.3 shows that while there were 4.7 persons of working age per elderly person in 2000, the Potential Support Ratio will decline to 3.5 in 2030 and 2.9 in 2050.
The new generation of senior citizens will meet their old age with more resources. The «new elderly» will have a better financial situation, better living conditions, a higher level of education and better health than any previous generation of elderly (ÆldreSagen 2001, Barstad 2006). Studies also show that in the future more elderly will have someone to live together with (Keilman 2010). Thus, an 80-year-old in 2030 will not be the same as an 80-year-old in 2010. On this basis, long-term planning should not only project the scenario involving problems and illnesses, but should also take into account the elderly population’s resources and ensure that these are used.
It is uncertain what the relationship between a longer life span and the needs for health services will be in the future. Three different hypotheses are possible:
A longer life will mean more good years of life because the period of serious loss of functionality will be about the same length as for today's elderly.
A longer life also will entail overall better health so that the period of serious loss of functionality will be shorter than today.
The period of serious loss of functionality will be longer.
Another relevant factor is that although the elderly of the future will have more health problems, they will also meet reduced functionality with more resources (Thorslund and Parker 2005).
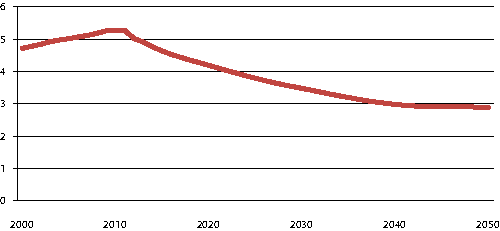
Figur 3.3 Number of persons of working age (16-66 years) per person 67 years and older. 2000-2050
Kilde: Statistics Norway 2010 Population projections, median alternative
3.2.3 The 25 per cent myth
It is claimed in many connections in the public debate that there is a need for 25 per cent coverage of nursing home beds as a percentage of the elderly 80 years of age and older, and that this is a government norm for nursing home coverage. This is a myth that is used in political exchanges, by special interest organisations and in local planning.
In fact, no such government norm exists. The figure of 25 per cent coverage also lacks any scientific basis and becomes particularly problematic when applied to individual municipalities.
The government has never established a norm or a minimum degree of coverage for 24-hour care spaces in nursing homes or residential care homes. It is the needs of the population in the individual municipality at any given point in time that determine how many people will be given 24-hour services in a nursing home, in a residential care home or in their own homes. There is a relatively wide variation in needs among the municipalities due to differences in the composition of the population and various local conditions. Contrary to claims, Report No. 31 (2001-2002) to the Storting, Avslutning av handlingsplan for eldreomsorgen («Conclusion of the Action Plan for Elderly Care») warned against applying such norms:
«The Government wishes to emphasise that the degrees of coverage should not be regarded as norms or minimum standards and that in this connection they should only be used as target figures for the action plan.»
The figure of 25 per cent is taken from Report No. 50 (1996-1997) to the Storting, Handlingsplan for eldreomsorgen («Action Plan for Elderly Care»), which states that «for the plan period 1998-2001, it is assumed that there will be a need for 24-hour care services provided in suitable dwellings corresponding to approximately 25 per cent of the population 80 years and older.»
The report emphasises that this is an estimate of the need for coverage on a nationwide basis provided that well-developed home care services and reasonable access to adapted dwellings are available. This applies to all age groups regardless of whether 24-hour care is provided in nursing homes, in residential care homes or in people’s own homes.
In other words, this figure is a 15-year-old estimate that was never meant to serve as a norm for the degree of coverage in the individual municipality, but which was used at the time as a basis for calculating the costs of the Action Plan for Elderly Care. This estimate, however, has begun to live a life of its own and gained status as a government norm in the public debate.
In recent years, it is primarily the number of recipients of municipal care services under the age of 67 that has risen. As a consequence, the degree of coverage viewed only in relation to the number of elderly over 80 years of age becomes less and less relevant. According to Statistics Norway, 24-hour coverage in nursing homes and residential care homes comprises 28 spaces per percentage of the population over 80 years of age, and is higher than anticipated when the Action Plan for Elderly Care was implemented.
3.2.4 The myth about informal care
The perception that public sector care displaces informal care and that the family withdraws if the public sector assumes responsibility remains widespread.
However, there is little evidence to suggest that families are failing in their caregiving duties. On the contrary, it appears that public sector care providers and volunteer informal caregivers cooperate with and complement each other. Informal care has proven to be dynamic and strong, and is more independent of public care services policy than presumed (Lingsom 1997). The level of stability in the extent of informal caregiving during the 20 to 30 years when this trend has been followed is striking (Daatland and Solem 2000, Rønning 2009). Nor is there evidence to suggest that the family withdraws when the public care system becomes involved by providing home care services. Although the welfare state has assumed the family’s previous obligations related to ageing, illness and disability, it does not appear that this has diminished family solidarity, as is often claimed (Langsether and Hellevik 2002).
The elderly who receive municipal home care services actually receive more help from their daughters and sons than the elderly who do not receive such services. The relationship between public and informal care is more cooperative than competitive in nature. A study of cooperation between public services and informal caregivers in the period from 1965 to 1995 shows that the amount of care provided to the elderly by family members remained stable rather than declined. Even though family members who provide care do so slightly less than before, there is much evidence to suggest that a larger number of people participate in this type of care provision (Lingsom 1997). More men participate, and the caregiving tasks are divided among several generations. Although the overall amount of informal care has remained at roughly the same level, the tasks are now divided among more recipients due to the major changes that have occurred in the age composition of the population.
However, families have less contact and provide less practical help when their elderly relatives live in nursing homes. It is easier for families and the public sector to share responsibility for caregiving tasks when the person in need of care lives at home or in a residential care home rather than in a nursing home (Lingsom 1997; Bogen and Høyland 2006). As a result, the expansion of home care services has ensured that the welfare state can continue to rely on, and cooperate with, the family in the provision of care services. The public home care services allow the family to provide assistance without having to assume the entire responsibility, leading to a kind of partnership with an informal distribution of tasks and responsibilities. This strengthens what the committee’s refers to as the «complementary hypothesis», meaning that under certain circumstances the public sector services and informal care can complement and strengthen each other. In contrast, some argue that the public care services replace, and in part compete with, informal caregiving, a situation described in the «substitution hypothesis» (Lingsom 1997; Daatland and Solem 2000; Daatland 1994).
The public care services have not expanded because families, friends and volunteers have failed their loved ones, but because there has been a need to move some of the caregiving arena out of the family and private sphere and to organise some of the caregiving tasks in a different way. The impetus for this was mainly to facilitate the inclusion of more women in working life in a period with a high demand for labour. This occurred simultaneously with a situation in which the needs of a rapidly increasing elderly population exceeded what families and volunteers could provide.
There used to be a widespread belief that the participation by women in working life would cause them to fail to perform their caregiving tasks in the family. In reality, there appears to be a positive correlation between participation in working life and caregiving. Working men and women provide as much care to their parents as those who are not employed.
In addition, the middle-aged women and men of the 60s generation have been shaped by the traditions and values of the society in which they grew up, and it seems unlikely that they will turn their backs on their parents. There appear to be small differences between the people who have made modern, individualistic choices regarding the family and working life and those who have made more traditional choices (Gautun 2003). However, there is reason to monitor whether the new generations will provide less care to the elderly due to their focus on self-realisation and individualisation or whether the amount of care they provide will remain stable or increase because it assumes new forms.
Next to the children of the elderly, it is primarily the grandchildren who provide practical help to their older relatives. A reciprocal relationship exists between the younger and older generations, whereby the assistance provided by younger adults to the elderly is counterbalanced by the financial and practical assistance younger adults in the establishment phase of their lives receive from their parents and grandparents. The potential for assistance inherent in family relationships remains great and must be viewed as a sign that the family ties are strong. Geographic proximity appears to be significant for the amount of help children provide to their parents. The closer children live to their parents, the more help the children provide to their parents (Gautun 1999).
Friends of the family also serve as important care providers throughout a person’s lifetime. In fact, friends often provide more assistance than siblings, including to the oldest age groups. Of people 80 years and older, three-fourths received practical help from their children in the past year, almost 40 per cent received help from their grandchildren and about one-fourth received help from friends (Langsether and Hellevik 2002).
While people have longer life spans they are also having fewer children. More and more people have both grandparents and great-grandparents who are still living, and many live to see both their grandchildren and great-grandchildren in their old age. Since practical help and contact are exchanged primarily through direct ascending and descending generations, it may be that more help from grandchildren will compensate for the lower number of siblings, nieces and nephews.
The «generation squeeze» experienced by the «sandwich generation» — that is, people with responsibility for providing care to their older parents as well as to their children — is limited in scope. If such a «generation squeeze» exists, it relates instead to people who care for their older parents and who themselves are grandparents providing care to their grandchildren (Hagestad 2003).
There are indications that formal and moral obligations are met through mutual commitments spawned through cooperation and the development of good mutual relations throughout one’s life (Gautun 1999 and 2003). More than before, people need to form their own networks and not just maintain the ones into which they were born. Perhaps close personal relationships and agreements between family members and friends can in the future compensate for and replace what is lost, should it turn out that the highly normative caregiving obligation vis-á-vis family and friends breaks down in modern society.
Close, strong personal relationships may therefore play a more important role in future care provision than pure moral obligation. This paves the way for more care providers both inside and outside the family circle and puts focus on people’s ability to build social relations. From this perspective, the opportunity for people to obtain informal support and care will depend more than before on solid social networks and the amount of «social capital» people bring with them into old age (Barstad 2006).
3.2.5 The illness myth
The municipal care services are developing a stronger health orientation, emphasising medication-based treatment, medical follow-up and nursing care. A report by the Norwegian Directorate of Health on care services in the past 20 years states that «Medical services are given priority over social services» (Norwegian Directorate of Health 2010a). The report points out that in-home nursing services account for most of the growth in the sector, while the number of recipients of practical assistance and housekeeping services has declined. Researchers note that in this way home care services have become more medically oriented (Romøren 2007):
«And it could be asked to what extent the home care services for the elderly have become medicalised at the expense of prevention and social and practical assistance» (Brevik 2010).
In addition, as homes for the aged have been phased out, medical care has taken on greater importance in institution-based care. This is a key feature in the development of the municipal care services in recent years, and is reflected in the professional groups that manage the sector and the expertise that is sought.
The committee is concerned about this trend as it relates to finding solutions to the future caregiving challenges.
People with reduced functionality are not necessarily patients nor are they sick. Ageing is not an illness either. It entails completely normal loss of functionality, greater practical obstacles, social factors and living conditions. The response must be to remove disabling barriers and to provide practical and personal help, assistance, activities, healthy meals, a satisfactory daily life, active prevention and early intervention.
Anxiety and grief may be an appropriate reaction to one’s own loss of functionality or to the loss of a loved one, but this need not manifest itself in illness. As a general rule, problems in human relationships or in a person’s relationship to their social and physical environment should also be solved before they result in illness.
A system which requires that people first have status as a patient before they are eligible to receive help with simple, basic tasks in daily life risks becoming involved too late. This implies a trend away from early intervention and prevention and towards the treatment of those patients with the greatest needs. This trend is probably an adaptation to a health service comprised of professional health personnel whose level of expertise in medical treatment is constantly being enhanced.
The field of «anti-ageing medicine» is growing rapidly throughout the world. The World Anti-Aging Academy of Medicine (WAAAM) was established in 1995 and states the following about its activities:
«Anti-aging and regenerative medicine are among the fastest-growing medical specialties throughout the world and are founded on the application of advanced scientific and medical technologies for the early detection, prevention, treatment, and reversal of age-related dysfunction, disorders, and diseases. It is a health-care model promoting innovative science and research to prolong the healthy life span in humans (WAAAM 2011).»
It is no longer just about wrinkle creams and liposuction, but also about plastic cosmetic surgery, hormone therapy, gene therapy, biotechnology, stem cell therapy and nanotechnology.
The committee cautions against turning age into an illness. It is true that the elderly fall ill more often than others and will need treatment. But ageing must also be allowed to be a natural part of life, both for the individual and in a societal context. Ageing is a biological, social and psychological process, and there is good reason to review and assess the cultural and social aspects of ageing, not least in relation to the role that the elderly should be assigned in the society of the future.
Similarly, one should avoid viewing people with reduced functionality as ill and instead help to dismantle physical, social and cultural barriers to their participation in working life and society at large.
3.3 Falls, loneliness and cognitive decline
Many people will experience accidental falls, loneliness and cognitive decline in the course of their lives. This may be because they are afflicted themselves or because someone they know is affected. The result is often a poorer general condition and reduced functionality. Much evidence suggests that these three factors are closely related and have a reciprocal impact on each other. A poorer general condition in one area often has consequences for the other areas, which in turn has ripple effects in other areas of life:
Unpleasant experiences with falls often result in a fear of falling again, leading to withdrawal, social isolation and inactivity.
A lack of social contact and stimulation can lead to more rapid cognitive decline.
Cognitive decline can lead to forgetfulness, reduced coordination and less attention to risk. This can in turn increase the likelihood of falling.
This «vicious circle» can be turned into a «circle of opportunity» with the help of preventive measures, innovative actions and appropriate, sensible use of technology.
The Irish Centre for Technology Research for Independent Living (TRIL) (see www.trilcentre.org) has shown how a poorer general condition in individuals, both physically and mentally, can result in:
Instability or a tendency to fall
Social isolation
Cognitive decline
The committee has chosen to use these three factors as a point of departure and illustration in its efforts to find new solutions and test them out. This applies to various types of living arrangements, technology, new work methods and ways of approaching the future caregiving challenges. In many ways, these factors also represent the various professional traditions in the health and social services sector, and show that interdisciplinary activities will be essential for developing new lines of thinking and innovative solutions in the care services.
3.3.1 Falls
Falls have many causes. They may be a pure accident or coincidence or they may be a sign of illness and a poor general condition. Falls and injuries from falls is one of the most common single reasons that the elderly are admitted to hospital. Each year about 30 per cent of all people over the age of 65 and 50 per cent of people over the age of 80 experience a fall. Roughly 10 000 people over the age of 65 break a hip due to a fall. Of these, eight of 10 are women. A broken hip causes excessive pain and a deterioration in quality of life, and the consequences are often so severe that they may lead to a long-term reduction in functionality, complications, accompanying diseases and death. Many never return to the same level of functionality they had prior to the break, becoming reliant on housekeeping services, in-home nursing care and stays in a nursing home (Skadeforebyggende Forum 2011; Sletvold 2010).
The risk factors for falls among the elderly are complex, but they can be classified into three categories: internal, external and risk exposure (Todd & Skelton, 2004). Internal factors include age, gender, whether a person lives alone, the use of medication, overall medical condition, reduced mobility/ability to walk, deficiency diseases, cognitive decline and diseases of the foot. External factors include poor lighting, slippery floors, uneven surfaces, footwear, clothing, inappropriate walking aids or other technical aids. Risk exposure involves the level of activity. Internal factors appear to be the most common among people over 80 years old, while external factors are most common among younger people.
A project in Nord-Trøndelag county analysed the more than 1 200 incidents of falls that occurred in the course of a year (Kjølstad, Pettersen, and Tvete, 2009). The data was taken from five municipalities and pertained to people over the age of 65. The findings showed that almost half of all falls occurred in the bedroom. In one-third of the cases the falls were caused by illness or dizziness, and in another third of the cases the person had tripped. Fifteen per cent had fallen from a chair or out of bed, and 13 per cent had fallen due to a slippery floor. Breaks and head injuries are among the most serious injuries from a fall.
Falls and injuries from falls are a health problem as well as a socioeconomic problem with a major negative impact on those affected. The consequences of a fall include not only the injury itself, but also the fear of falling again, leading to inactivity with accompanying decline in functionality, social isolation, reduced quality of life and, in the most serious cases, death. Many fall without injuring themselves physically, but they experience the same insecurity and fear of falling again and injuring themselves. In many cases, this leads to a reduction in physical activity and social withdrawal.
The risk of falling can be prevented and reduced through various forms of physical activity, physical training, rehabilitation and medical treatment. One example of a prevention measure is the «Fall Project» in Trondheim. The project is a cooperative effort between several players who work in an active, targeted way to prevent falls among the elderly (Sletvold 2010).
3.3.2 Loneliness
Loneliness is the feeling of a lack of desired contact with others. The person who is lonely has less contact with others or the contact is less meaningful than he or she would like. Thus the person’s desire for contact, and not only the contact itself, is of significance. Being lonely is therefore not the same as being alone or isolated, living alone, having few friends or have little social interaction. Loneliness and «aloneness» are two different conditions. Nonetheless, people with only a few contacts say more often that they are lonely than people with many contacts (Thorsen & Clausen 2009).
Only about one per cent of the population says that they do not have any good friends. The elderly lack good friends to a somewhat greater degree than younger people, but the number of people between 60 and 79 years of age who say they lack good friends has declined, from seven per cent in 1980 to three per cent in 2007 (Barstad A. 2009). About one in 10 states that they do not have any good friends in the place where they live. This figure remained stable from 1987 to 2007. Elderly, single men comprise the largest group with a relatively unsatisfactory friendship situation. They have a low level of education and are often without jobs. They may receive a disability pension or work at home, and they tend to be in poor health and have financial difficulties.
Women state more often than men that they feel lonely (Barstad A 2000). Men have fewer close friends than women have, and they often say that their spouse is their only close relationship. Loneliness is most widespread among the oldest age groups, among those 80 years and older and in the 70-79 year age group, and the difference in perceived loneliness between women and men increases with age. Women are usually married to older men, they experience the loss of a spouse more often, they live alone more often, they live longer and they have more health concerns. All of these factors may play a role in why women tend to feel lonely more often than men.
Young people often blame their loneliness on their own personal qualities, and this affects their self-esteem to a greater extent than the elderly, who are more likely to attribute their loneliness to external factors such as the death of their spouse or closest friends. The group that feels the least lonely is young adults, people in the establishment phase of life and established adults.
Feelings of loneliness are also associated with poor health. Poor health may lead to loneliness, and feelings of loneliness may lead to poor health. It is known that loneliness can cause depression, insomnia, tension, anxiety and despair (Luanaigh and Lawlor 2008). Three times as many people who say they are in poor health have feelings of loneliness as compared with people who say they are in excellent or very good health (Tornstam 1988, Lunaigh and Lawlor 2008). There appears to be a stronger correlation between loneliness and mental health than between loneliness and physical health (Thorsen and Solem 2005).

Figur 3.4 Percentage who state that they do not have anyone outside of their own family in whom they can confide. 1980-2007
Kilde: Statistics Norway, A. Barstad. Living conditions survey and LOGG 2007, Statistics Norway and Norwegian Social Research (NOVA)
3.3.3 Cognitive decline
It is generally understood that cognitive functioning refers to the ability to comprehend and obtain information from the world around us, store it, and plan and act on the basis of this information. Even ordinary tasks, such as engaging in conversation, require complex interaction between many different thought processes. Although there are individual differences in people’s natural cognitive abilities, there is good reference data to indicate what may be considered normal cognitive functioning. In order to apply the term «cognitive decline», the deficiency must be significant enough as to have a negative impact on the person’s ability to tackle daily challenges and demands. Thus, cognitive decline is a concept viewed in relation to the individual person’s life situation (Follesø 2010).
Mild cognitive decline may be described as a gradual reduction in cognitive performance, and commonly occurs with increasing age. In some cases, a slightly more pronounced cognitive decline occurs than is expected with age, even though this does not fulfil the criteria for a diagnosis of dementia. This may often be manifested in an experienced or proven memory problem, and it may have many different causes.
Neurological diseases caused by pathological changes in the central nervous system are often classified according to the physical symptoms they produce. However, many feel that their illness is not limited to the physical aspect, but that a decline in cognition is a crucial aspect of their overall condition.
Dementia is an umbrella term for several different brain diseases that often occur in old age and result in cognitive decline. The most important symptom or defining feature of dementia is memory loss. People afflicted with dementia have difficulties maintaining learned skills and mastering daily tasks. Some people develop changes in their personality such as a lack of insight and poor judgment. Other frequent symptoms are anxiety, depression, suspicion, delusions and obsessive-compulsive behaviour.
Currently in Norway about 70 000 people have some form of dementia, and it is estimated that 10 000 people are stricken with the disease each year. Studies show that only half of them are examined and diagnosed (Ministry of Health and Care Services 2007). Activity and social contact may enhance the quality of life for people with dementia and cognitive decline, and to some extent delay the development of the disease and reduce the need for treatment with medication.
Conclusion
Falls, loneliness and cognitive decline constitute a «vicious circle» which has major ramifications for the people afflicted and for society at large. Preventive measures that help to remove the risk factors or reduce the consequences of falls, loneliness and cognitive decline will therefore be a good investment in the future.
The committee has chosen to use these three factors as the point of departure and illustration for its efforts to find new solutions and test them out. Falls involve a person’s relationship to the physical environment. Loneliness involves the person as a social being and the relationship between people. Cognitive decline involves the brain and the person as a biological being. Together they represent crucial challenges that call for interdisciplinary cooperation between the medical, social and technical fields in order to find new solutions in which the use of new technology and new housing solutions, combined with activity and treatment, can prevent falls from occurring and loneliness from arising or reduce the consequences of increasing cognitive decline. The committee refers to the discussion of this in chapter 5 and onward of this report.
3.4 Borderless care services
The committee has chosen to refer to the internationalisation of care services as the «seventh challenge». In the future people will cross municipal boundaries and national borders more often to obtain health and care services, and health and social care workers and companies that provide such services will operate in several different countries.
3.4.1 Patients and users without borders
Today more and more patients and users are crossing national borders to obtain treatment and participate in recreational activity and physical training. Some combine their holidays with dental treatment or an eye operation in Asia; others travel to the Mediterranean coast for parts of the year for recreation and for health-related reasons. Norway is not the only country where this is happening. Throughout the world, patient and user flows are becoming internationalised across regions and national borders. It is easy to obtain information from the Internet, and the new generation of senior citizens has more resources than before and appears to be more mobile. Certain countries address some of their caregiving challenges by sending people in need of care services to other countries where labour is less costly and access to care workers is simpler (Isaksen 2005).
3.4.2 International labour market
The labour market, including health and social care personnel, is becoming internationalised, and care workers are crossing national borders to provide care to other people’s families abroad.
«The global care chain»
An increasing proportion of the world’s population is migrating from one country to another. A large part of the labour migration that occurs among women is related to what could be called the «care deficit» in the rich part of the world. The export of care workers has therefore already become a major growth industry for poor countries.
On the one hand, women are employed as au pairs or maids by families caught in a time crunch between employed work and caring for their children and elderly relatives. Many of these women support their own children and families in their home country by taking care of other people’s children and families abroad. This situation has been termed the «global care chain» (Hochschild 2001, Isaksen 2001, Yeates 2005). Some also get married in another country, and after some time they bring their mothers with them to take care of their children. These «transnational grannies» expand the global care chain even further. Part of this picture includes illegal immigrants who are exploited as undocumented maids and home assistants, some of whom are forced into prostitution (Isaksen 2001).
«Care drain»
On the other hand, there are health and social care professionals who have the opportunity to emigrate to Western countries in order to help meet the demand for health and care personnel in hospitals and elderly care facilities. They come from India, Thailand and the Philippines to the US, Europe and the Middle East, or they come from countries in Eastern Europe to Western Europe (Isaksen 2005). In this way, the «care drain» becomes one aspect of the «brain drain», a situation in which expertise moves from the areas where the need is greatest to areas where demand and the ability to pay are greatest.
Boks 3.1 Sunrise Senior Living
Sunrise Senior Living operates 365 «senior living communities» with almost 40 000 residents in most US states as well as in Canada, England and Germany. The company offers:
Independent Living Assisted Living Alzheimer's Care
Nursing & Rehabilitative Care
Hospice Care
Short-term Stays
Kilde: http://www.sunriseseniorliving.com/
3.4.3 International providers
At the same time, service providers are crossing national borders. Norwegian municipalities are establishing nursing homes, physical rehabilitation services and residential care homes in the Mediterranean countries, or entering into agreements with others that provide these services. And the thousands of Norwegians who have become residents or long-term tourists of Spain are working to expand Norwegian involvement in social measures and care services along the Spanish coast.
The relationship between health and climate is given as a main motivation factor for the rather extensive emigration to and long-term tourism in Spain. Individuals suffering from rheumatism and asthma experience especially positive health effects, such as less pain, a simpler daily life, better training opportunities and less use of medication. Although only scarcely one-fourth of Norwegians in Spain say they would travel home to Norway if they were to become severely ill or injured, they nonetheless harbour worries about finding themselves in such a situation and are working actively for the establishment of good care services with assistance from their home country. The question then becomes whether it is easier, less expensive and better, not only for the users but also for their home municipalities in Norway, to finance or establish care services in Spain, as many would like (Helset et al. 2004, Sørbye et al. 2004).
A growing number of service providers offer recreational activities, physical training services and care services in this international market. Both major international humanitarian organisations and more commercial players offer everything from short-term, traditional spa stays to long-term stays in institutions or permanent relocation to senior living communities. These communities are targeted at people 55 years and older and offer activities, daytime programmes, practical and personal assistance, separate nursing home facilities and special services for people with dementia (Barstad 2007).
In Norway, Nordic companies such as Norlandia Care and Alleris provide home care services and institution-based services to various user groups, and Adecco, the world’s largest staffing agency, has been involved in the operation of several nursing homes.
Boks 3.2 Two small projects on the Norwegian-Swedish border
Gränsprojekt
The EU-funded INTERREG project Midt-Skandinavisk Regionprosjekt encompasses the Frostviken region in Strömsunds municipality and the Hotagen region in Krokoms municipality in Jämtland county, both in Sweden, and Lierne and Røyrvik municipalities in Nord-Trøndelag county in Norway. The project promotes industrial development, cooperation on and development of public service production, and the removal of border-related barriers as a means of reversing the negative population trend in the region. The cooperative project also entails health and care services. See http://www.gransprojekt.eu/
Gränslös omsorg («Borderless care»)
Gränslös omsorg is a cooperative project between Inari municipality in Sweden and Sør-Varanger municipality in Norway which aims to develop new, innovative business models for cooperation on elderly care and home care services that extend across national borders.
Kilde: See www.interregnord.com/